If Fat Loss Feels “Stubborn”, Read This
This is my gift especially for woman as we approach Woman’s Day.
Stubborn Fat Isn’t Imaginary – It’s Biological
But before we even get to the science, let’s name the real fear. It’s not just about weight. It’s this quiet thought:
“What if I can’t trust myself to make good food decisions — for my body and my family?”
No matter what you try, it feels like you either gain weight… or you overthink every bite. You second-guess. You research. You start again.
And somewhere in the background is the worry that you’ll never just eat in a normal, sustainable way — without feeling deprived, confused or slightly on edge.
If you’ve been carrying shame, frustration, or that subtle sense of being “less than” because this feels harder than it should…
It’s time to change the conversation. Because once you understand what’s really happening, everything shifts. And I say that not from theory — but from experience. Despite my nutrition degree, there were years when I felt exactly the same.
So before we go any further, let me say this clearly:
You are not failing.
You’ve been navigating a science that has been evolving in real time.
A Quick Trip Back to the 1960s
In the 1960s, scientists discovered something called hormone sensitive lipase — HSL.
Here’s what that means in simple terms: Inside your fat cells is a tiny mechanism that helps unlock stored fat when your body needs energy. Think of it like a key that opens your stored fuel tank. For years, the thinking was simple: If you eat less, the key turns, the fat comes out.
Sounds straightforward enough…
Except… for many women, it didn’t feel straightforward. It led to shame, secret eating, frantic choices, stop start with one trend after another, supplements, metabolism boosters, starvation, sadness and lack of confidence…
1990s: The First Crack in the Story
Then researchers discovered that fat cells themselves can become insulin resistant.
You probably already know insulin is the hormone that helps manage blood sugar and fat storage. When fat cells become resistant, they stop responding properly. And if fat cells aren’t responding properly, they don’t release stored fat efficiently either.
That was a turning point.
Because suddenly the conversation shifted from:
“Why aren’t you trying hard enough?”
To:
“Something is happening at a cellular level.”
2000s: Fat Isn’t Just Storage
This is when we learned that fat tissue isn’t passive. When everything is working correctly it’s active. It sends signals. It releases hormones.
But when fat cells enlarge too much — from years of consistent overconsumption (from any source, not just fat) — they can become oxygen deprived. This is called hypoxia and here’s what happens:
Low oxygen → inflammation → more insulin resistance → more dysfunction.
In plain English: Overfilled fat cells become stressed. And stressed fat cells don’t quietly cooperate when you diet.
They dig their heels in and defend the status quo.
2010s: “Adipose Dysfunction” Becomes Real
By the 2010s, the evidence was overwhelming.
We now know that overfilled fat cells:
- Stop responding properly to adrenaline (a fat-burning signal)
- Slow down fat release
- Can stall fat loss — even when someone is genuinely eating less!
This was the science that finally validated millions of women’s (including my own) lived experience. It wasn’t laziness. It wasn’t weakness. It wasn’t lack of discipline or even under reporting! It was biology adapting.
As always, energy balance still matters.
But the condition of the fat tissue matters too. And no one explained that properly.
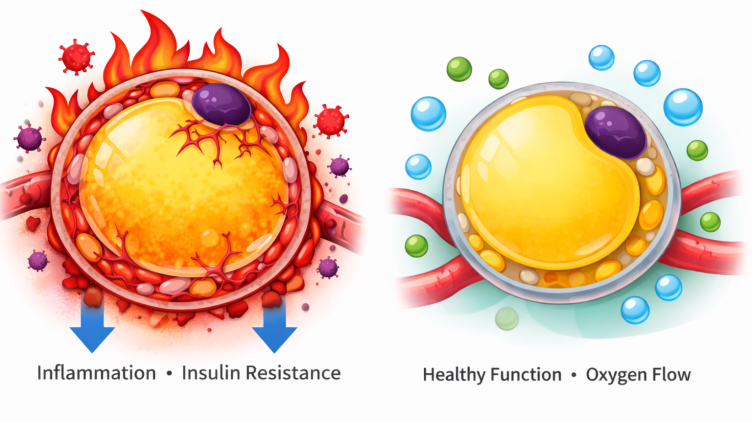
Generated by Chat GPT
2021 Onwards: Muscle Changes the Conversation
Then something fascinating emerged.
When you do resistance training — strength work, not just steady cardio — your muscles release tiny chemical messengers.
Those messengers help fat cells respond better to fat-burning signals.
In other words: Muscle improves communication which is why strength training changes bodies differently. Not because it “tones”.
But because it restores signalling.
And Here’s Where the Shame Ends
If you’ve been stuck in cycles of:
Restrict. Try harder. Blame yourself. Start again Monday.
Pause.
Your body hasn’t betrayed you. It has adapted to long-term conditions.
Fat-loss resistance isn’t a moral issue. It’s a biological state.
That doesn’t mean effort doesn’t matter.
It means the strategy matters!
One Final (Important) Caveat
Everything you’ve just read is human biology.
Not just female biology.
- Fat cells enlarge.
- They can become inflamed.
- They can become insulin resistant.
- They can become resistant to releasing fat.
That happens in men too.
But here’s why this matters on International Women’s Day.
Women have disproportionately carried the cultural shame around weight.
From teenage magazines to “bounce back” headlines… From post-pregnancy pressure to menopause invisibility… From being told to eat less, be smaller, try harder.
When fat loss stalled, the story was personal failure. Not cellular adaptation. Men experience fat-loss resistance too.
But women have been far more likely to internalise it as a character flaw. And that’s the part we’re retiring.
This conversation is for anyone whose body feels stubborn.
It’s especially for the women who have quietly blamed themselves for decades.
Biology explains difficulty. It doesn’t remove responsibility but it absolutely removes shame.
What You Take Away Today
- Overconsumption of energy — from any source — enlarges fat cells over time.
- Enlarged fat cells can become stressed, inflamed and resistant.
- That resistance makes fat release slower — even in a calorie deficit.
- Muscle restores communication.
- Sleep, stress and inflammation matter.
- Punishment is not the answer.
The elementary truths are still the same: What’s changed is our understanding of why it can feel harder than the magazines, supplementary programmes and fitness fast programmes promised.
- You are not incapable.
- You are not defeated.
- And you absolutely can take back control.
But control comes from understanding — not shame.
Because Real Nutrition Matters.
Niki Kerr is a qualified nutritionist, an award-winning writer and behaviour-change specialist. Bringing a thought-leader lens to Food, Nutrition and modern weight loss (including GLP-1 medications) with an evidenced focus on what actually works in real life: nourishment, consistency, and behaviour change that sticks.

